Travel Clinic
Our Travel Service
Our travel clinic is based at our Fleetwood Health Centre branch. We offer the same service that you would expect from a dedicated travel clinic. We can administer vaccinations and supply anti-malarial medication. We offer tailored travel advice and benefit from stocking a wide range of travel goods such as first aid kits , anti-diarrhoea medicine, travel sickness medicines, mosquito nets / repellents and much more.
Travel Vaccinations and Anti-Malaria Medication
Following an assessment of your itinerary, type of travel and length of stay, we can offer advice on which vaccinations and anti-malarials are most suitable for your trip. More information on the vaccinations and the diseases they help prevent can be found below. If you require any further information about your intended destination and the precautions you should take then please visit the NHS Fit for Travel website
Cholera
A vaccination is available to protect against cholera when travelling, although most people won't need it because food and water hygiene precautions are usually enough to prevent infection.
Vaccination is usually only recommended for travellers to areas where cholera is widespread, particularly for aid workers and people who are likely to have limited access to medical services.
The cholera vaccine is usually available on the NHS, but this can vary. It's also available through private prescription from a private travel clinic.
The vaccine
The cholera vaccine is given as a drink, where the vaccination ingredients are mixed with water. You should avoid eating, drinking or taking oral medication for an hour before and after having the vaccination.
For adults and children over the age of six, two doses of the vaccine are needed to protect against cholera for two years. After this, a booster is required if you continue to be at risk.
Children who are two to six years of age will need to have three doses of the vaccine. This will protect them for six months. After this, they will need to have a booster if they continue to be at risk.
All the doses must be taken one to six weeks apart. If more than six weeks passes between doses, you'll need to start the full vaccination course again.
Ideally, the vaccination course should be completed at least one week before travelling.
The cholera vaccine isn't recommended for children under two years of age, because it's not clear how well it works in this age group.
Side effects and precautions
After having the cholera vaccine, less than 1 in 100 people will experience short-term symptoms similar to a mild stomach upset, such as abdominal pain, diarrhoea and nausea. Severe reactions are very rare.
Most people can have the vaccination safely, but you should tell the doctor or nurse before being vaccinated if you:
- have a high temperature (fever) or stomach upset
- are pregnant or think you might be pregnant
- are breastfeeding
- have a condition, or are receiving treatment, that affects your immune system
In these circumstances, you may still be able to have the vaccine if you're at a high risk of getting cholera, but your doctor or nurse may need to check with a travel medicine specialist before giving it to you. The vaccination may need to be delayed if you're unwell with a fever or upset stomach.
You shouldn't have the vaccine if you've had an allergic reaction to the cholera vaccine or any of the vaccine components in the past.
What is malaria?
Malaria is a tropical disease which is transmitted by mosquitos. To become infected all it takes is one bite.
Malaria can cause a serious risk to your health, and can even prove fatal, if it isn't diagnosed and treated properly. If you are travelling to high risk areas it is important that you protect yourself against this disease.
If contracted, malaria can present with the following symptoms;
-
Fever
-
Chills and sweats
-
Headaches
-
Muscle pains
-
Diarrhoea and vomiting
Symptoms can appear as soon as seven days after being infected but may take much longer to present.
If the symptoms present and you are in a malaria risk area or have just returned from an ‘at risk’ area medical advice must be sought immediately.
What causes malaria?
Malaria is caused by a parasite known as Plasmodium. Many different types exist but only certain strains cause the disease in humans.
The parasite is passed from mosquito to humans when a bite occurs, this often is more prevalent at dusk and through the night. When the bite occurs, the parasite passes into the bloodstream causing infection.
In what countries am I at risk of catching malaria?
It is not possible to contract malaria in the UK, however 100 countries around the world contain areas in which malaria-carrying mosquitos are present. Affected areas include:
-
Large areas of Africa and Asia
-
Central and South America
-
Haiti and The Dominican Republic
-
Parts of the Middle east
-
Pacific Islands
How can I protect myself against malaria?
At our travel clinic, we have everything you need to protect yourself and stay safe when travelling around the globe.
-
We can advise you on which countries you are at risk of contracting malaria in
-
Speak to one of our pharmacists about some of the simple steps you can take to prevent the bites happening. We can provide simple day-to-day travel advice as well as recommending products such as insect repellents
-
We use the latest guidance to advise on which malaria prevention tablets are best for your travel schedule. We have a range of malaria prevention tablets available and can supply these following a consultation with one of our pharmacists without a prescription and without delay!
Hajj and Umrah Recommendations
The risk of malaria is low in Mecca and Medina and antimalarial prophylaxis is not advised while in either city. However, the journey between them passes through an area of high risk for malaria. The journey takes six hours by road. If it is undertaken during the daytime, in an air conditioned vehicle from which mosquitoes can be excluded, the risk of malaria is very low and it is reasonable to practice bite avoidance only.
Overview
Rabies is a rare but very serious infection of the brain and nerves. It's usually caught from the bite or scratch of an infected animal, most often a dog.
Rabies is found throughout the world, particularly in Asia, Africa and Central and South America. It's not found in the UK except in a small number of wild bats.
It's almost always fatal once symptoms appear, but treatment before this happens is very effective. There's also a vaccine for people at risk of being infected.
Rabies vaccination
You should consider getting vaccinated against rabies if:
- you're travelling to an area where rabies is common and you plan to stay for a month or more or there's unlikely to be quick access to appropriate medical care
- you're travelling to an area where rabies is common and you plan to do activities that could put you at increased risk of exposure to animals with rabies, such as running or cycling
Visit your GP or a travel clinic if you think you may need the vaccine. It's sometimes free, but most people have to pay.
Even if you've been vaccinated, you should still take precautions to avoid coming into contact with rabies if you're travelling in an area where rabies is found and get medical advice straight away if you've been bitten or scratched.
A few people may need the rabies vaccine because they could come into contact with rabies through their work. If you think this applies to you, speak to your occupational health department.
Read more about the rabies vaccination.
How to avoid being bitten or scratched
All mammals (including monkeys) can carry rabies, but it's most common in:
- dogs
- bats
- raccoons
- foxes
- jackals
- cats
- mongooses
They can spread the infection if they bite or scratch you, or in rare cases if they lick an open wound or their saliva gets into your mouth or eyes. Rabies isn't spread through unbroken skin or between people.
While travelling in an area where rabies is a risk:
- avoid contact with animals – some infected animals may behave strangely, but sometimes there may be no obvious signs they're infected
- avoid touching any dead animals
If you're travelling with a child, make sure they're aware of the dangers and that they should tell you if they've been bitten, scratched or licked by an animal. Check them for any wounds if they come into contact with an animal.
For information about areas where rabies is a risk, see:
What to do if you've been bitten or scratched
If you've been bitten or scratched by an animal in an area with a risk of rabies:
- immediately clean the wound with running water and soap for several minutes
- disinfect the wound with an alcohol- or iodine-based disinfectant and apply a simple dressing, if possible
- go to the nearest medical centre, hospital or GP surgery as soon as possible and explain that you've been bitten or scratched
If this happens while you're abroad, get local medical help immediately. Don't wait until you've returned to the UK.
If you've already returned to the UK without getting medical advice, it's still a good idea to get help – even if it's been several weeks since you were bitten or scratched.
It's unlikely that you've been infected, but it's best to be safe. Post-exposure treatment is nearly 100% effective if it's started before any symptoms of rabies appear.
Treatment after a bite or scratch
If you've been bitten, scratched or licked by an animal that might have rabies, you may need specialist medical treatment to stop you getting rabies. This is called post-exposure treatment.
Post-exposure treatment involves:
- cleaning and disinfecting the wound
- a course of the rabies vaccine – you'll need to have five doses over a month if you haven't been vaccinated before, or two doses a few days apart if you have
- in some cases, a medicine called immunoglobulin given into and around the wound – this provides immediate but short-term protection if there's a significant chance you've been infected
Treatment should be started as soon as possible, ideally within a few hours of being bitten or scratched.
But it's often safe to delay treatment until the next day if the vaccine and/or immunoglobulin need to be specially ordered in by your doctor.
Symptoms of rabies
Without treatment, the symptoms of rabies will usually develop after 3-12 weeks, although they can start sooner or much later than this.
The first symptoms can include:
- a high temperature (fever) of 38C (100.4F) or above
- a headache
- feeling anxious or generally unwell
- in some cases, discomfort at the site of the bite.
Other symptoms appear a few days later, such as:
- confusion or aggressive behaviour
- seeing or hearing things (hallucinations)
- producing lots of saliva or frothing at the mouth
- muscle spasms
- difficulty swallowing and breathing
- inability to move (paralysis)
Once symptoms appear, rabies is almost always fatal. In these cases, treatment will focus on making the person as comfortable as possible.
Rabies in the UK
The UK has been rabies-free since the beginning of the 20th century, with the exception of a rabies-like virus in a species of wild bat called Daubenton's bats.
This has only been found in a few bats and the risk of human infection is thought to be low. People who regularly handle bats are most at risk.
There has only been one recorded case of someone catching rabies from a bat in the UK. It's also rare for infected bats to spread rabies to other animals.
But if you find an injured or dead bat, do not touch it. Wear thick gloves if you need to move it. Call the Bat Conservation Trust helpline on 0345 1300 228 for advice.
Overview
A hepatitis A vaccine is available for people at a high risk of infection.
Symptoms of hepatitis A
The symptoms of hepatitis A develop, on average, around four weeks after becoming infected, although not everyone will experience them.
Symptoms can include:
- feeling tired and generally unwell
- joint and muscle pain
- a high temperature (fever)
- loss of appetite
- feeling or being sick
- pain in the upper-right part of your tummy
- yellowing of the skin and eyes (jaundice)
- dark urine and pale stools
- itchy skin
The symptoms will usually pass within a couple of months.
Read more about symptoms of hepatitis A.
When to get medical advice
See your GP for advice if:
- you have symptoms of hepatitis A – a blood test can usually confirm whether you have the infection
- you might have been exposed to the hepatitis A virus recently but you don't have any symptoms – treatment given early on may be able to stop the infection developing
- you think you might need the hepatitis A vaccine – your GP can advise you about whether you should have the vaccine (see below)
Although hepatitis A isn't usually serious, it's important to get a proper diagnosis to rule out more serious conditions with similar symptoms, such as hepatitis C or cirrhosis (scarring of the liver).
It may also be necessary to test your friends, family and any sexual partners, in case you've spread the infection to them.
How you can get hepatitis A
Hepatitis A is most widespread in parts of the world where standards of sanitation and food hygiene are generally poor, such as parts of Africa, the Indian subcontinent, the Far East, the Middle East, and Central and South America.
You can get the infection from:
- eating food prepared by someone with the infection who hasn't washed their hands properly or washed them in water contaminated with sewage
- drinking contaminated water (including ice cubes)
- eating raw or undercooked shellfish from contaminated water
- close contact with someone who has hepatitis A
- less commonly, having sex with someone who has the infection (this is particularly a risk for men who have sex with men) or injecting drugs using contaminated equipment
Someone with hepatitis A is most infectious from around two weeks before their symptoms appear until about a week after the symptoms first develop.
Read more about the causes of hepatitis A.
Vaccination against hepatitis A
Vaccination against hepatitis A isn't routinely offered in the UK because the risk of infection is low for most people.
It's only recommended for people at an increased risk, including:
- close contacts of someone with hepatitis A
- people planning to travel to or live in parts of the world where hepatitis A is widespread, particularly if levels of sanitation and food hygiene are expected to be poor
- people with any type of long-term (chronic) liver disease
- men who have sex with other men
- people who inject illegal drugs
- people who may be exposed to hepatitis A through their job – this includes sewage workers, staff of institutions where levels of personal hygiene may be poor (such as a homeless shelter) and people working with monkeys, apes and gorillas
The hepatitis A vaccine is usually available for free on the NHS for anyone who needs it.
Read more about the hepatitis A vaccine.
Treatments for hepatitis A
There's currently no cure for hepatitis A, but it will normally pass on its own within a couple of months. You can usually look after yourself at home.
While you're ill, it's a good idea to:
- get plenty of rest
- take painkillers such as paracetamol or ibuprofen for any aches and pains – ask your GP for advice about this, as you may need to take lower doses than normal or avoid certain medications until you've recovered
- maintain a cool, well-ventilated environment, wear loose clothing, and avoid hot baths or showers to reduce any itching
- eat smaller, lighter meals to help reduce nausea and vomiting
- avoid alcohol to reduce the strain on your liver
- stay off work or school and avoid having sex until at least a week after your jaundice or other symptoms started
- practise good hygiene measures, such as washing your hands with soap and water regularly
Speak to your GP if your symptoms are particularly troublesome or haven't started to improve within a couple of months. They can prescribe medications to help with itchiness, nausea or vomiting, if necessary.
Read more about treating hepatitis A.
Outlook for hepatitis A
For most people, hepatitis A will pass within two months and there will be no long-term effects. Once it passes, you normally develop life-long immunity against the virus.
For around 1 in every 7 people with the infection, the symptoms may come and go for up to 6 months before eventually passing.
Life-threatening complications such as liver failure are rare, affecting less than 1 in every 250 people with hepatitis A. People most at risk include those with pre-existing liver problems and elderly people.
If liver failure does occur, a liver transplant is usually needed to treat it.
Overview
A hepatitis B vaccine is available for people at high risk of the condition.
Symptoms of hepatitis B
Many people with hepatitis B won't experience any symptoms and may fight off the virus without realising they had it.
If symptoms do develop, they tend to occur two or three months after exposure to the hepatitis B virus.
Symptoms of hepatitis B include:
- flu-like symptoms, including tiredness, a fever, and general aches and pains
- loss of appetite
- feeling and being sick
- diarrhoea
- tummy (abdominal) pain
- yellowing of the skin and eyes (jaundice)
These symptoms will usually pass within one to three months (acute hepatitis B), although occasionally the infection can last for six months or more (chronic hepatitis B).
When to get medical advice
Hepatitis B can be serious, so you should get medical advice if:
- you think you may have been exposed to the hepatitis B virus – emergency treatment can help prevent infection if given within a few days of exposure
- you have symptoms associated with hepatitis B
- you're at a high risk of hepatitis B – high-risk groups include people born in a country where the infection is common, babies born to mothers infected with hepatitis B, and people who have ever injected drugs
You can go to your local GP surgery, drug service, genitourinary medicine (GUM) clinic or sexual health clinic for help and advice.
A blood test can be carried out to check if you have hepatitis B or have had it in the past. The hepatitis B vaccine may also be recommended to reduce your risk of infection.
Treatments for hepatitis B
Treatment for hepatitis B depends on how long you've been infected for:
- If you've been exposed to the virus in the past few days, emergency treatment can help stop you becoming infected.
- If you've only had the infection for a few weeks or months (acute hepatitis B), you may only need treatment to relieve your symptoms while your body fights off the infection.
- If you've had the infection for more than six months (chronic hepatitis B), you may be offered treatment with medicines that can keep the virus under control and reduce the risk of liver damage.
Chronic hepatitis B often requires long-term or lifelong treatment and regular monitoring to check for any further liver problems.
How hepatitis B is spread
The hepatitis B virus is found in the blood and bodily fluids, such as semen and vaginal fluids, of an infected person.
It can be spread:
- from a mother to her newborn baby, particularly in countries where the infection is common – read more about hepatitis B in pregnancy
- within families (child to child) in countries where the infection is common
- by injecting drugs and sharing needles and other drug equipment, such as spoons and filters
- by having sex with an infected person without using a condom
- by having a tattoo, body piercing, or medical or dental treatment in an unhygienic environment with unsterilised equipment
- by sharing toothbrushes or razors contaminated with infected blood
Hepatitis B is not spread by kissing, holding hands, hugging, coughing, sneezing, or sharing crockery and utensils.
Preventing hepatitis B
A vaccine that offers protection against hepatitis B is available for all babies born in the UK on or after August 1 2017. It is also available for people at high risk of the infection or complications from it.
This includes:
- babies born to hepatitis B-infected mothers
- close family and sexual partners of someone with hepatitis B
- people travelling to a part of the world where hepatitis B is widespread, such as sub-Saharan Africa, east and southeast Asia, and the Pacific Islands
- families adopting or fostering children from high-risk countries
- people who inject drugs or have a sexual partner who injects drugs
- people who change their sexual partner frequently
- men who have sex with men
- male and female sex workers
- people who work somewhere that places them at risk of contact with blood or body fluids, such as nurses, prison staff, doctors, dentists and laboratory staff
- people with chronic liver disease
- people with chronic kidney disease
- prisoners
- people receiving regular blood or blood products, and their carers
The hepatitis B vaccine is given to infants as part of the routine child vaccination schedule and to those who are at high risk of developing the infection.
You do not need to pay for the vaccine if your child is eligible to receive it as part of the routine child vaccination schedule or if born to a hepatitis B-infected mother. Others may have to pay for it.
Read more about hepatitis B vaccination.
Outlook for hepatitis B
The vast majority of people infected with hepatitis B in adulthood are able to fight off the virus and fully recover within one to three months. Most will then be immune to the infection for life.
Babies and children with hepatitis B are more likely to develop a chronic infection. Chronic hepatitis B affects around:
- 90% of babies with hepatitis B
- 20% of older children with hepatitis B
- 5% of adults with hepatitis B
Although treatment can help, there's a risk that people with chronic hepatitis B could eventually develop life-threatening problems such as scarring of the liver (cirrhosis) or liver cancer.
Overview
There's currently no cure for Japanese encephalitis. Treatment involves supporting the functions of the body as it tries to fight off the infection. This usually requires the person being admitted to hospital, so they can be given fluids, oxygen and medication to treat any symptoms.
Symptoms
Most people infected by the Japanese encephalitis virus have either no symptoms, or mild, short-lived symptoms, which are often mistaken for flu.
However, around 1 in every 250 people who become infected with Japanese encephalitis develop more severe symptoms, as the infection spreads to the brain. This usually happens 5-15 days after infection and symptoms can include:
- high temperature (fever)
- seizures (fits)
- stiff neck
- confusion
- inability to speak
- uncontrollable shaking of body parts (tremor)
- muscle weakness or paralysis
Up to one in every three people who develop these more serious symptoms will die as a result of the infection.
In those who survive, these symptoms tend to slowly improve. However, it can take several months to make a full recovery and up to half of those who do survive are left with permanent brain damage. This can lead to long-term problems such as tremors and muscle twitches, personality changes, muscle weakness, learning difficulties and paralysis in one or more limbs.
When to seek medical advice
You should seek immediate medical advice if you have any of the symptoms of Japanese encephalitis and have recently visited, or are still in, an area where the infection is found.
GOV.UK has information about who to contact when you need immediate medical help abroad. If you're already back in the UK, see your GP.
Your GP or the healthcare professional treating you will ask about your symptoms, where you've been travelling, what you did on your trip and what vaccinations you've had. If necessary, they may carry out a blood test to see if you have an infection.
How common is Japanese encephalitis?
It's very rare for travellers visiting risk areas to be affected by Japanese encephalitis. It's estimated that less than one in a million travellers develop Japanese encephalitis in any given year.
The people most at risk are those who live and work in rural areas where the condition is widespread. Around 75% of cases involve children under the age of 15.
Find out more about the causes of Japanese encephalitis and the countries and activities which have a higher risk of catching the disease.
The World Health Organization (WHO) estimates there are around 68,000 cases of Japanese encephalitis worldwide each year.
Preventing Japanese encephalitis
The best way to prevent Japanese encephalitis is to be vaccinated against the infection before you visit a part of the world where there's a risk of catching it. The risk is greater if you're planning to visit rural areas or go hiking or camping.
The vaccine, which is usually only available privately, gives protection against Japanese encephalitis in more than 9 out of 10 people who receive it.
Even if you've been vaccinated, you should still take precautions to reduce your risk of being bitten by an infected mosquito, such as:
- sleeping in rooms with close-fitting gauze over the windows and doors – if you're sleeping outside, use mosquito nets that have been impregnated with an insecticide
- covering up with long-sleeved tops, trousers and socks
- applying a good-quality insect repellent to exposed areas of skin
Read more about preventing Japanese encephalitis.
Overview
If someone else eats food or drinks water that's been contaminated with a small amount of infected faeces or urine, they can become infected with the bacteria and develop typhoid fever.
Read more about the causes of typhoid fever.
Who's affected?
Typhoid fever is most common in parts of the world that have poor sanitation and limited access to clean water (at the bottom of this page is a list of high-risk areas).
Worldwide, children are thought to be most at risk of developing typhoid fever. This may be because their immune system (the body's natural defence against infection and illness) is still developing. However, children with typhoid fever tend to have milder symptoms than adults.
Typhoid fever is uncommon in the UK, with an estimated 500 cases occurring each year. In most of these cases, the person developed the infection while visiting relatives in Bangladesh, India and Pakistan. However, you're also at risk of developing the infection if you visit Asia, Africa and South America.
Signs and symptoms of typhoid fever
Common symptoms of typhoid fever include:
- a high temperature that can reach 39-40C (103-104F)
- stomach pain
- headache
- constipation or diarrhoea
If typhoid fever isn't treated, the symptoms will continue to get worse over the following weeks and the risk of developing potentially fatal complications will increase.
Read more about the symptoms of typhoid fever and the complications of typhoid fever.
How typhoid fever is treated
Typhoid fever requires prompt treatment with antibiotics. If diagnosed at an early stage, the infection is likely to be mild and can usually be treated at home with a 7- to 14-day course of antibiotic tablets.
More serious cases of typhoid fever usually require admission to hospital, so antibiotic injections can be given.
With prompt antibiotic treatment, most people will start to feel better within a few days and serious complications are very rare. Deaths from typhoid fever are now virtually unheard of in the UK.
If typhoid fever isn't treated, it's estimated that up to one in five people with the condition will die. Some of those who survive will have complications caused by the infection.
Read more about treating typhoid fever.
Typhoid fever vaccination
In the UK, two vaccines are available that can provide some protection against typhoid fever. These involve either having a single injection or taking three capsules over alternate days.
Vaccination is recommended for anyone planning to travel to parts of the world where typhoid fever is widespread (see below). It's particularly important if you're planning to live or work closely with local people.
However, as neither vaccine offers 100% protection, it's also important to follow some precautions when travelling. For example, you should only drink bottled or boiled water, and avoid foods that could potentially be contaminated.
Read more about the typhoid fever vaccination.
High-risk areas
The areas with the highest rates of typhoid fever are:
- the Indian subcontinent
- Africa
- South and South East Asia
- South America
- the Middle East
- Europe
- Central America
Overview
Yellow fever vaccination
The yellow fever vaccine is recommended if you're travelling to:- an area where yellow fever is found
- a country that requires you to have a certificate proving you've been vaccinated against yellow fever
Where yellow fever is found
Yellow fever is found in:- most of sub-Saharan Africa (the area below the Sahara desert)
- most of South America
- parts of Central America
- parts of the Caribbean
- Travel Health Pro: maps of where yellow fever is found
- Travel Health Pro: country information
How yellow fever is spread
Yellow fever is a virus spread by mosquito bites. You can't get it from close contact with someone who has it. The mosquitoes that spread the infection are found in towns and rural areas. They mainly bite during the day. If you're travelling to an area where yellow fever is found, try to avoid being bitten – even if you've been vaccinated – as mosquitoes can also spread other serious illnesses, such as malaria and dengue. You can do this by using mosquito nets, wearing clothes that cover your arms and legs, and using insect repellent containing 50% DEET. Read more about how to prevent insect bites.Symptoms of yellow fever
The first symptoms of yellow fever usually develop three to six days after being infected. They include:- a high temperature (fever) of 38C (100.4F) or above
- a headache
- feeling sick or vomiting
- muscle pain and backache
- your eyes being sensitive to light
- loss of appetite and feeling generally unwell
- yellowing of the skin and eyes (jaundice)
- bleeding from the mouth, nose or eyes
- vomiting blood or blood in poo
When to get medical help
See a doctor straight away if you get symptoms of yellow fever while travelling in an area where the infection is found. If you get symptoms after recently returning from one of these areas, contact your GP or NHS 111 for advice as soon as possible. Tell them exactly where you've been travelling, if you think you've been bitten by a mosquito, and what symptoms you have. You may need to have a blood test to check for the infection.Treatments for yellow fever
There's no cure for yellow fever, but the symptoms can be treated while your body fights off the infection. Most people make a full recovery after three or four days. Painkillers such as paracetamol or ibuprofen can help lower your temperature and relieve aches or pains in the meantime. Also drink plenty of fluids to avoid dehydration. If you have more serious symptoms, you may need to go into hospital for close monitoring and treatment of your symptoms until you're feeling better.Diphtheria vaccination
Diphtheria is rare in the UK because babies and children are routinely vaccinated against it.
When childhood diphtheria vaccinations are given
Travel vaccination
The best way to avoid diphtheria while travelling is to be fully vaccinated against it.
If you're travelling to a part of the world where diphtheria is widespread, you may need a booster vaccination if you were last vaccinated against it more than 10 years ago.
Diphtheria is found in many areas, including:
- Asia
- the South Pacific
- the Middle East
- eastern Europe
- the Caribbean
Places considered to be high risk can change over time. For up-to-date information about the area you're visiting, check the TravelHealthPro country guides.
For foreign travel, you may be able to get a combined vaccine against diphtheria, tetanus and polio free on the NHS. Ask at your GP surgery.
How diphtheria is spread
Diphtheria is highly contagious. It's spread by coughs and sneezes, or through close contact with someone who's infected.
You can also get it by sharing items – such as cups, cutlery, clothing or bedding – with an infected person.
Symptoms of diphtheria
- a thick grey-white coating at the back of your throat
- a high temperature (fever) of 38C or above
- feeling sick
- sore throat
- headache
- swollen glands in your neck
- difficulty breathing and swallowing
If it affects your skin (cutaneous diphtheria), it can cause:
- pus-filled blisters on your legs, feet and hands
- large ulcers surrounded by red, sore-looking skin
Get urgent medical help if you have symptoms of diphtheria and:
- you're in an area of the world where the infection is widespread
- you've recently returned from somewhere where the infection is widespread
- you've been in close contact with someone who has diphtheria
Diphtheria needs to be treated quickly in hospital to help prevent serious complications, such as breathing difficulties or heart problems.
Treatments for diphtheria
The main treatments are:
- antibiotics to kill the diphtheria bacteria
- medicines that stop the effects of the harmful substances (toxins) produced by the bacteria
- thoroughly cleaning any infected wounds if you have diphtheria affecting your skin
Treatment usually lasts 2 to 3 weeks. Any skin ulcers usually heal within 2 to 3 months but may leave a scar.
People who have been in close contact with someone who has diphtheria may also need to take antibiotics or may be given a dose of the diphtheria vaccination.
How you get tetanus
Tetanus bacteria can survive for a long time outside the body, and are commonly found in soil and the manure of animals such as horses and cows. If the bacteria enter the body through a wound, they can quickly multiply and release a toxin that affects the nerves, causing symptoms such as muscle stiffness and spasms. The bacteria can get into your body through:- cuts and scrapes
- tears or splits in the skin
- burns
- animal bites
- body piercings, tattoos and injections
- eye injuries
- injecting contaminated drugs
Symptoms of tetanus
The symptoms of tetanus usually develop 4 to 21 days after infection. On average, they start after around 10 days. The main symptoms include:- stiffness in your jaw muscles (lockjaw), which can make opening your mouth difficult
- painful muscle spasms, which can make breathing and swallowing difficult
- a high temperature (fever) of 38C (100.4F) or above
- sweating
- a rapid heartbeat
When to get medical advice
Contact your GP or visit your nearest minor injuries unit if you're concerned about a wound, particularly if:- it's a deep wound
- there's dirt or something inside the wound
- you haven't been fully vaccinated, or you're not sure if you have
How tetanus is treated
If your doctor thinks you could develop tetanus but you haven't had any symptoms yet, they'll clean your wounds and give you an injection of tetanus immunoglobulin. They may also give you a dose of the tetanus vaccine if you haven't been fully vaccinated in the past. Tetanus immunoglobulin is a medication containing antibodies that kill the tetanus bacteria. It provides immediate, but short-term, protection from tetanus. If you develop symptoms of tetanus, you'll usually need to be admitted to a hospital intensive care unit (ICU), where you may be given a number of different treatments. These could include tetanus immunoglobulin, antibiotics, and medication to relieve muscle stiffness and spasms. Most people who develop symptoms of tetanus eventually recover, although it can take several weeks or months.Tetanus vaccination
A tetanus vaccination is given as part of the NHS childhood vaccination programme. The full course of the vaccination requires five injections, usually given on the following schedule:- The first three doses are given as part of the 6-in-1 vaccine at 8, 12 and 16 weeks for all babies born on or after August 1 2017.
- A booster dose is given as part of the 4-in-1 pre-school booster at age three years and four months.
- A final booster is given as part of the 3-in-1 teenager booster at age 14.
Tetanus travel jab
Tetanus is found throughout the world, so you should ideally make sure you're fully vaccinated before travelling abroad. Contact your GP surgery for advice if you're planning on travelling abroad and haven't been fully vaccinated against tetanus, or you're going to an area with limited medical facilities and your last vaccine dose was more than 10 years ago. If you've never had a tetanus vaccination before, you may be advised to have as many of the three initial doses of the vaccine as possible before you leave (there should be one-month gaps between each dose) and complete the full course when you return. If you've been partly or fully vaccinated, a tetanus shot is usually still recommended as a precaution if you're travelling to an area with limited medical facilities and your last dose of the vaccine was more than 10 years ago. You'll be offered another 3-in-1 teenage booster. This additional booster, which also protects against diphtheria and polio, is usually free on the NHS. Read more about travel vaccinations.Symptoms of polio
About 95% of people with polio won't have any symptoms and will fight off the infection without even realising they were infected. A small number of people will experience a flu-like illness 3 to 21 days after they're infected. Symptoms can include:- a high temperature (fever) of 38C (100.4F) or above
- a sore throat
- a headache
- abdominal (tummy) pain
- aching muscles
- feeling and being sick
Long-term problems caused by polio
Although polio often passes quickly without causing any other problems, it can sometimes lead to persistent or lifelong difficulties. About 1 in every 200 people with the infection will have some degree of permanent paralysis, and others may be left with problems that require long-term treatment and support. These can include:- muscle weakness
- shrinking of the muscles (atrophy)
- tight joints (contractures)
- deformities, such as twisted feet or legs
How do you get polio?
You can become infected with the polio virus if you come into contact with the poo (faeces) of someone with the infection, or with the droplets launched into the air when they cough or sneeze. You can also get the infection from food or water that's been contaminated with infected poo or droplets. If the virus gets into your mouth, it travels to your throat and bowels, where it starts to multiply. In some cases, it can also get into the bloodstream and spread to the nervous system. The virus can be spread by someone with the infection from about a week before any symptoms develop, until several weeks afterwards. Infected people who don't have any symptoms can still pass polio on to others. There have been rare cases where polio has been caused by being vaccinated with a live version of the polio virus. This is no longer a risk in the UK because the vaccine used nowadays contains an inactive version of the virus.Where is polio found?
As a result of routine vaccination programmes, polio has been largely wiped out in most parts of the world. Areas declared polio-free by the World Health Organization (WHO) include Europe, the Americas, the western Pacific region and, most recently, southeast Asia. But polio is found in some places. It's still a significant problem in Afghanistan, Nigeria and Pakistan, and there's a potential risk of infection in other parts of Africa and some Middle Eastern countries. You can use the country guide on the Travel Health Pro website to check if there's a risk of getting polio in a country you plan to visit.Treating polio
There's currently no cure for polio. Treatment focuses on supporting bodily functions and reducing the risk of long-term problems while the body fights off the infection. This can include bed rest in hospital, painkillers, breathing support and regular stretches or exercises to prevent problems with the muscles and joints. If you're left with long-term problems as a result of a polio infection, you'll probably need ongoing treatment and support. This may include physiotherapy to help with any movement problems, devices such as splints and braces to support weak limbs or joints, occupational therapy to help you adapt to any difficulties, and possibly surgery to correct any deformities.Polio vaccination
The polio vaccination is offered as part of the NHS routine childhood vaccination programme. It's given by injection in 5 separate doses. These are normally given at:- 8, 12 and 16 weeks of age – as part of the 6-in-1 vaccine
- 3 years and 4 months of age – as part of the 4-in-1 (DTaP/IPV) pre-school booster
- 14 years of age – as part of the 3-in-1 (Td/IPV) teenage booster
Temporary precautions for travellers
As the result of an increase in worldwide cases of polio in early 2014, the WHO issued temporary additional travel recommendations for people visiting countries where polio is found. Depending on where you intend to travel, what you'll be doing there and how long you're staying for, you may now be advised to have a booster polio vaccination before travelling if you haven't had one in the past 12 months. Some of the countries where there's risk of infection will require proof of vaccination before you're permitted to travel elsewhere. If you don't have this, you may be given a booster dose before departing.Check if you could be at risk of TBE
The risk of getting TBE while travelling is very low. Ticks that spread it are found in:- most of Europe (not the UK)
- Russia
- parts of China and Japan
You can get vaccinated against TBE if you're at risk
Consider having the TBE vaccine if you're visiting a country where the infection is found and you're planning to do outdoor activities when you get there. Two injections of the vaccine can protect you for about a year. A third injection can protect you for about 3 years. You need to have the first injection at least 1 month before travelling.How to avoid tick bites
Try to avoid being bitten by ticks in places where TBE is found, even if you've been vaccinated. To reduce the risk of being bitten:- cover your skin while walking outdoors and tuck your trousers into your socks
- use insect repellent on your clothes and skin – products containing DEET are best
- stick to paths whenever possible
- wear light-coloured clothing so ticks are easier to spot and brush off
How to spot and remove ticks
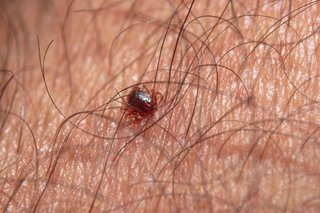
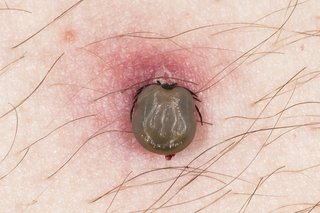

- Use fine-tipped tweezers or a tick removal tool. You can buy these from some pharmacies, vets and pet shops.
- Grasp the tick as close to your skin as possible.
- Slowly pull upwards, taking care not to squeeze or crush the tick. Dispose of it when you've removed it.
- Clean the bite with antiseptic or soap and water.
See a doctor if:
- you've been bitten by a tick or visited an area in the past month where infected ticks are found
- flu-like symptoms – such as feeling hot and shivery, headaches, aching muscles or feeling sick, or
- a circular red rash
Go to hospital if you or someone else:
- gets a stiff neck and a severe headache
- gets pain when looking at bright lights
- has a seizure (fit)
- has a change in behaviour – such as sudden confusion
- develops weakness or loss of movement in part of the body

Travel Health
Sunscreen – Depending on your destination (even for winter sports) sunblock with an SPF factor of at least 15 is essential and it is important for the sun cream to have a broad-spectrum to protect against both UVA and UVB rays.
Aftersun – The sun's rays can dehydrate the skin so it is important to keep it at its best. Aftersun helps to rehydrate the skin and undo the damage the sun has caused and is particularly important in sunburn.
Antiseptic and first aid – Small scrapes and scratches have an increased risk of infection in hot and humid climates so it is important to take either a small bottle of antiseptic or antiseptic wipes in case problem occurs. Bandages, plasters and tweezers may also be useful.
Antihistamines – Itching and inflammation caused by bites can spoil your holiday. Over-the-counter antihistamines, gels and creams can help relieve these symptoms. Some steroid creams may also be appropriate for those nastier bites.
Insect repellent – As well as considering the risk of malaria at your holiday destination and taking appropriate medical advice, other measures to help prevent getting bites in the first place include nets, plug-in repellents and DEET-containing insect repellent.
Rehydration Sachets - These can be essential to help replace fluids and salts that are lost from diarrhoea, vomiting and the problems associated with too much sun. These sachets help you stay hydrated much better than drinking regular water.
Antibacterial hand gel – When you don’t have access to soap and water antibacterial hand gels can kill germs especially before eating and after going to the bathroom.
Common medications – When travelling abroad you can’t always guarantee the quality of the medication you receive so make sure to pack the essentials, such as paracetamol, in addition to any regular prescription medications that you take.
So, for FREE personalised travel health advice and your travel health essentials, don't delay call us on 01253 770103 or book here

All the prices for the vaccinations and anti-malarials we offer can be found below, please note the cost is per dose. Some vaccinations require a number of doses for the course to be fully effective. All the information on required number of doses will be given after our initial assessment of your travel itinerary We strongly recommend completing the full course of any vaccination. Incomplete courses may result in reduced immunity and/or reduced length of immunity, however we can administer single vaccinations as part of a course started/to be completed elsewhere.
| Vaccination | Cost |
| Cholera | £65 |
| Diptheria, Tetanus, Polio | £30 |
| Hepatitis A | £47 |
| Hepatitis A & Typhoid | £70 |
| Hepatitis B | £45 |
| Hepatitis A & B | £60 |
| Rabies | £60 |
| Typhoid(injection) | £30 |
| Typhoid(oral) | £30 |
| Japanese Encephalitis | £95 |
| Meningitis ACWY | £70 |
| MMR | £32 |
| Tick Bourne Encephalitis |
£62 |
| Yellow Fever (no certificate) |
£55 |
| Yellow Fever (with certificate) |
£70 |

